AI Overview (60 words)
Lifestyle stress affects the skin through hormones, inflammation, sleep disruption, and daily habits. Breakouts, rashes, dullness, flare-ups, and accelerated aging often reflect what’s happening internally. This guide explains how stress shows up on your skin, why it happens biologically, and which evidence-based habits, routines, and professional options actually help restore skin health.
Stress isn’t just something you feel—it’s something your skin reveals. For many Americans, long work hours, constant digital exposure, financial pressure, poor sleep, and irregular routines quietly shape the condition of their skin. Breakouts that won’t resolve, redness that comes and goes, unexpected rashes, or skin that suddenly looks dull and tired are often signals of lifestyle stress rather than product failure.
Dermatologists increasingly recognize the skin as a mirror of internal balance. Research cited by organizations like the American Academy of Dermatology shows that psychological and physical stressors can directly disrupt skin barrier function, immune response, and oil regulation. Understanding how stress shows up on your skin—and what actually helps—can prevent unnecessary treatments, wasted money, and frustration.
The Skin–Stress Connection: What’s Happening Beneath the Surface
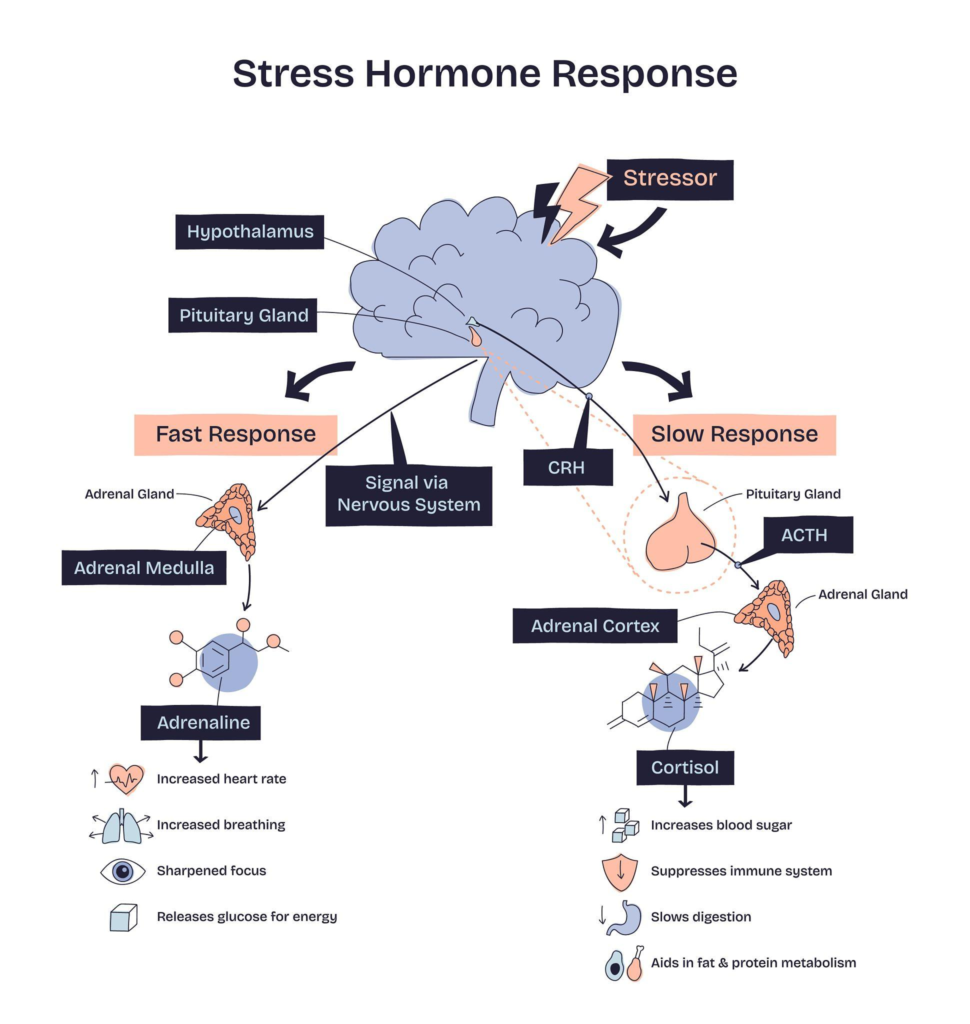
When you experience stress, your body releases cortisol and other stress hormones. These chemicals are designed to help you respond to threats, but when stress becomes chronic, they start interfering with normal skin processes.
Elevated cortisol increases oil production, weakens the skin barrier, slows healing, and fuels inflammation. Over time, this makes skin more reactive and less resilient. According to data from the Centers for Disease Control and Prevention, chronic stress is also associated with sleep disruption, immune imbalance, and metabolic changes—all of which influence skin health.
Stress doesn’t cause one universal skin problem. Instead, it amplifies your skin’s natural tendencies. Oily skin may break out more easily. Dry or sensitive skin may become irritated or inflamed. Conditions you already have may flare more often.
Stress-Related Skin Issues Americans Commonly Experience
Acne That Feels Sudden or Persistent
Stress-related acne often appears along the jawline, chin, or cheeks in adults who didn’t struggle with acne in their teens. Cortisol stimulates sebaceous glands, leading to clogged pores and inflammation. Stress can also worsen acne indirectly by disrupting sleep, encouraging comfort eating, or leading to inconsistent skincare routines.
This is why “doing everything right” with products doesn’t always fix the issue. Without addressing stress patterns, topical solutions may only provide temporary relief.
Eczema, Psoriasis, and Inflammatory Flare-Ups
Inflammatory skin conditions are particularly sensitive to emotional stress. Studies published in dermatology journals consistently show that stress can trigger flare-ups by altering immune responses and increasing inflammatory markers.
Patients often notice cycles: symptoms worsen during deadlines, caregiving stress, or major life transitions, then calm during periods of rest or routine stability.

Rosacea and Facial Redness
Stress-induced blood vessel dilation contributes to flushing and persistent redness. For rosacea-prone individuals, emotional stress can be as powerful a trigger as heat, alcohol, or spicy foods.
Stress management often becomes a critical component of rosacea treatment—not just an optional add-on.
Dullness, Uneven Tone, and Premature Aging
Stress slows cell turnover and collagen production. Over time, this contributes to:
- A tired, grayish appearance
- Fine lines that deepen faster
- Loss of elasticity and firmness
Poor sleep compounds the effect. Research from sleep medicine studies shows that people who consistently sleep fewer than six hours experience accelerated skin aging and slower recovery from environmental damage.
Hair and Scalp Changes
Stress-related skin effects don’t stop at the face. Many Americans notice increased scalp sensitivity, dandruff, itching, or even stress-related hair shedding (telogen effluvium). These changes often appear two to three months after a high-stress period, making the connection easy to miss.
Lifestyle Stressors That Quietly Damage Skin Health
Stress isn’t always dramatic. The most damaging forms are often low-grade and chronic.
Common contributors include long workdays with minimal movement, irregular meals, excessive caffeine, constant screen exposure, and lack of recovery time. Financial pressure, caregiving responsibilities, and social isolation can also elevate baseline stress levels even when life seems “manageable.”
Environmental stress matters too. Pollution exposure, artificial lighting, and temperature-controlled indoor air all challenge the skin barrier when combined with psychological stress.
Why Skincare Alone Often Isn’t Enough
Many people respond to stress-related skin issues by switching products repeatedly. While a solid skincare routine is important, products can’t override chronic cortisol elevation or sleep deprivation.
Over-exfoliation, harsh actives, and constant product experimentation can worsen stress-compromised skin. In these cases, the skin needs stabilization, not stimulation.
Dermatologists frequently recommend simplifying routines during high-stress periods to support barrier repair and reduce inflammation.
What Actually Helps: Evidence-Based Strategies
Restore the Skin Barrier First
A healthy barrier reduces sensitivity, inflammation, and moisture loss. Look for moisturizers with ceramides, glycerin, and niacinamide. Avoid fragranced products if stress has made your skin reactive.
Consistency matters more than complexity. A gentle cleanser, moisturizer, and daily sunscreen form the foundation.
Improve Sleep Quality, Not Just Quantity
Sleep is when skin repairs itself. Even one week of poor sleep can increase transepidermal water loss and redness.
Helpful strategies include maintaining consistent sleep times, reducing screen exposure before bed, and keeping bedrooms cool and dark. These changes often improve skin appearance within weeks.
Address Stress at the Nervous System Level
Stress management doesn’t require drastic lifestyle changes. Small, repeatable habits are often more effective:
- Short daily walks
- Controlled breathing exercises
- Limiting late-night work emails
- Scheduling recovery time like you would appointments
Studies in psychodermatology show that even modest reductions in perceived stress can improve inflammatory skin conditions.
Support Skin Through Nutrition
Stress depletes key nutrients involved in skin repair, including zinc, magnesium, and B vitamins. Diets high in ultra-processed foods can worsen inflammation.
Whole foods, adequate protein, omega-3 fatty acids, and hydration support both stress regulation and skin resilience. Many dermatologists now consider nutrition part of comprehensive skin care.
Know When to Seek Professional Help
If stress-related skin issues persist, a board-certified dermatologist can help identify underlying patterns and recommend targeted treatments. Mental health support can also play a role—especially when skin issues themselves become a source of stress.

Frequently Asked Questions
Can stress really cause skin problems?
Yes. Chronic stress alters hormone levels, immune function, and skin barrier integrity, all of which directly affect skin health.
Why does my skin flare up during busy weeks?
Deadlines, poor sleep, irregular meals, and cortisol spikes combine to increase inflammation and oil production.
Does stress-related acne need different treatment?
Often, yes. Treatment may focus more on calming inflammation and supporting barrier repair rather than aggressive acne actives.
Can reducing stress improve skin without changing products?
In many cases, yes. Improved sleep and stress management alone can noticeably improve skin tone and texture.
Is stress aging my skin faster?
Research suggests chronic stress accelerates collagen breakdown and slows repair, contributing to premature aging.
Why does my eczema worsen when I’m anxious?
Stress triggers immune responses that increase inflammation and itch perception.
Does exercise help stress-related skin issues?
Moderate exercise improves circulation, sleep quality, and stress regulation, all of which benefit skin.
How long does it take for skin to recover from stress?
Some improvements appear within weeks, but full recovery can take months depending on severity and consistency.
Should I change my skincare routine during stressful periods?
Simplifying and focusing on barrier repair is often more effective than adding new products.
Skin as a Stress Signal, Not a Failure
Your skin isn’t betraying you—it’s communicating. Breakouts, rashes, or dullness are often early signals that your lifestyle needs adjustment, not punishment. When stress is addressed alongside skincare, improvements tend to be more sustainable and less frustrating. Healthy skin is rarely about perfection; it’s about resilience.
Key Signals Worth Noticing
- Sudden skin changes often reflect internal stress
- Chronic issues usually require lifestyle support, not just products
- Consistency and recovery matter more than intensity
- Skin improves when stress is managed systemically

